Connect With Us
Blog

Blisters on the Feet
Blisters are a common ailment of people who wear shoes that are either too tight or rub against the feet in an uncomfortable way. Knowing the basics of blisters is important for understanding how they are formed and what treatments should be used for them.
A blister on the foot, or any other part of the body, is a small pocket that is filled with fluid. It usually forms on the upper layer of the skin because these layers are loose enough to allow a blister to form. The most common fluid in a blister is just a clear, watery-like fluid that usually isn’t cause for concern. However, blisters can fill up with blood if they are deep enough and pus if they have become infected with bacteria.
Blisters almost always form on the feet due to shoes rubbing up against the foot, where the friction causes blisters. These can occur after you have walked for a long period of time or when your shoes do not fit you properly. Your feet are also more prone to blisters if they are moist, so keeping them dry and clean is one preventative step you can take.
Preventing infection should be the number one concern when treating blisters, as well as relieving the pain they can cause. Using a bandage to cover up the blister will help it heal and prevent bacteria from entering it. New skin will form under the blister and eventually cause it to pop. You can also take a sterilized pin and try to pop it yourself.
If the blister is filled with pus or blood, seeking treatment from a doctor is ideal. Antibiotics may need to be taken in order to completely eliminate the bacteria inside the blister. See a doctor to have an antibiotic prescribed.
The best way to treat blisters is to prevent them all together. Keeping your feet dry and making sure that your shoes fit properly are just two of the steps you can take to prevent blisters. Shoes that are too tight or shoes that are too loose and allow your feet to slide in them will cause blisters. Applying a bandage to an area where you think a blister is about to form is another way you can prevent them.
Taking Care of Diabetic Feet
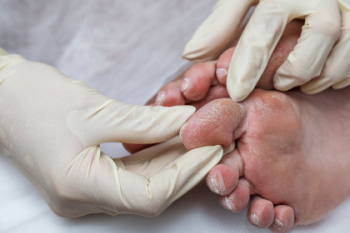 Diabetes is a chronic condition characterized by elevated blood glucose levels due to the body's inability to produce or effectively use insulin. This condition can lead to various complications, particularly affecting the feet. High blood sugar can damage nerves and reduce blood flow, increasing the risk of foot problems. Common issues include neuropathy, which can cause loss of sensation, and peripheral artery disease, leading to poor foot circulation. These complications can result in infections, ulcers, and, in severe cases, amputations if not properly managed. To avoid foot problems, individuals with diabetes should maintain good blood sugar control, inspect their feet daily for cuts, blisters, or changes in skin color, and keep their feet clean and moisturized. Choosing proper footwear is important, as wearing ill-fitting shoes and socks can cause pressure points and sores. If you have diabetes, it is suggested that you see a podiatrist regularly to monitor and manage your foot health.
Diabetes is a chronic condition characterized by elevated blood glucose levels due to the body's inability to produce or effectively use insulin. This condition can lead to various complications, particularly affecting the feet. High blood sugar can damage nerves and reduce blood flow, increasing the risk of foot problems. Common issues include neuropathy, which can cause loss of sensation, and peripheral artery disease, leading to poor foot circulation. These complications can result in infections, ulcers, and, in severe cases, amputations if not properly managed. To avoid foot problems, individuals with diabetes should maintain good blood sugar control, inspect their feet daily for cuts, blisters, or changes in skin color, and keep their feet clean and moisturized. Choosing proper footwear is important, as wearing ill-fitting shoes and socks can cause pressure points and sores. If you have diabetes, it is suggested that you see a podiatrist regularly to monitor and manage your foot health.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact one of our podiatrists from Lexington Foot and Ankle Center, PSC. Our doctors can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
- Routinely inspect your feet for bruises or sores.
- Wear socks that fit your feet comfortably.
- Wear comfortable shoes that provide adequate support.
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions please feel free to contact our offices located in Harrodsburg, Frankfort, Georgetown, and Lexington, KY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Diabetic Foot Conditions
According to the American Diabetes Association (ADA), diabetes is a condition that affects approximately 23.6 million Americans. Around 750,000 new cases are diagnosed each year, and the disease’s most common form, Type 2 diabetes, makes up for 90 to 95 percent of these cases. Type 2 diabetes is especially prevalent among older Americans, those who are obese, and those who lead sedentary lifestyles.
Complications of the disease may lead to several foot and ankle-related conditions. The loss of nerve sensation, or neuropathy, can cause diabetics to lose feeling at the bottom of the feet and therefore leave them unaware of pain, pressure, and heat. Decreased circulation is another complication of diabetes that can slow down the healing of wounds and injuries; this can lead to the development of foot ulcers.
To prevent foot ulcers from forming, diabetics should examine their feet every day for small cuts and wear shoes that curtail pressure. Constant monitoring for the risk factors associated with ulcer formation can allow for early detection and therefore lessen the possibility of ulcers or, even worse, amputation. The removal of calluses and ingrown toenails should be left to the podiatrist to avoid improper removal and possible infection.
Diabetic patients may also experience foot deformities due to complications in their feet, such as limited joint mobility, muscle atrophy, and decreased fat padding. These complications can increase pressure in certain areas of the foot, which in turn can cause certain deformities, such as hammertoe, to form. Another deformity, Charcot foot, develops due to the collapsing of microfractures in the bones of the feet. The resulting deformity is a foot that is flattened and wider in appearance.
To help minimize pressure and prevent the development of these diabetes-related foot and ankle conditions, your podiatrist may consider using orthotics or special shoes. Charcot foot may be treated using walkers, custom orthotic insoles, or non-weight-bearing or rigid weight-bearing casts or braces. In more serious cases, surgery may be considered to treat more developed deformities. Ulcers can be further cared for with the help of proper diet, medication to control glucose, intensive wound care, and infection treatment.
High Heels and Women’s Foot Problems

High heels are a staple in many women's wardrobes, with about 40 percent wearing them daily. However, the fashionable choice often comes with a painful price. Three quarters of women wearing high heels experience foot pain regularly. The height of the heel and the narrowness of the toe box are the main culprits. High heels often force toes into unnatural positions, that may lead to bunions, which are bumps along the inside of the big toe, and hammertoes, where toes become bent at the middle joint. Over time, these conditions can worsen, causing significant discomfort and permanent changes in foot structure. High heels also can contribute to tight calf muscles, which may result in plantar fasciitis and Achilles tendonitis. To avoid these issues, select shoes with a proper fit, ensuring that your toes have adequate space to move. For those already suffering, treatments include toe pads, separators, and in severe cases, surgery. If you are experiencing foot pain from high heels, it may be time to reconsider your footwear choices. For guidance with foot problems, it is suggested that you schedule an appointment with a podiatrist for an exam and treatment options.
High heels have a history of causing foot and ankle problems. If you have any concerns about your feet or ankles, contact one of our podiatrists from Lexington Foot and Ankle Center, PSC. Our doctors can provide the care you need to keep you pain-free and on your feet.
Effects of High Heels on the Feet
High heels are popular shoes among women because of their many styles and societal appeal. Despite this, high heels can still cause many health problems if worn too frequently.
Which Parts of My Body Will Be Affected by High Heels?
- Ankle Joints
- Achilles Tendon – May shorten and stiffen with prolonged wear
- Balls of the Feet
- Knees – Heels cause the knees to bend constantly, creating stress on them
- Back – They decrease the spine’s ability to absorb shock, which may lead to back pain. The vertebrae of the lower back may compress.
What Kinds of Foot Problems Can Develop from Wearing High Heels?
- Corns
- Calluses
- Hammertoe
- Bunions
- Morton’s Neuroma
- Plantar Fasciitis
How Can I Still Wear High Heels and Maintain Foot Health?
If you want to wear high heeled shoes, make sure that you are not wearing them every day, as this will help prevent long term physical problems. Try wearing thicker heels as opposed to stilettos to distribute weight more evenly across the feet. Always make sure you are wearing the proper shoes for the right occasion, such as sneakers for exercising. If you walk to work, try carrying your heels with you and changing into them once you arrive at work. Adding inserts to your heels can help cushion your feet and absorb shock. Full foot inserts or metatarsal pads are available.
If you have any questions please feel free to contact our offices located in Harrodsburg, Frankfort, Georgetown, and Lexington, KY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Effect of High Heels on the Feet
High heels are uncomfortable, but many women sacrifice comfort to be stylish. There are many problems that stem from wearing high heels, however these issues can be avoided by wearing proper shoes.
Heels are bad because they push your weight forward toward the fall of the foot. The higher the heel is, the more weight and pressure get shifted. This process causes the back to hyperextend backwards to counterbalance which may cause pain in the leg, hip, and back. Consequently, major posture problems may occur, and these issues may eventually become permanent.
Wearing high heels is one of the leading cause of ingrown toenails. Heels create a great deal of pressure on the big toenails which disrupts proper toenail growth. This may eventually lead to the big toenail growing into the skin. Another common problem that stems from high heels is bunions. If bunions go untreated, they can cause serious scar tissue to form along with severe pain.
However, there are ways to minimize the harmful risks associated with wearing heels. You should try to massage and stretch your legs and feet after wearing heels for an extended time. Stretching helps prevent the Achilles tendons and calf muscles from becoming too tight. A good substitute for heels are platforms which provide a better surface area to evenly distribute the body’s weight.
If you are experiencing any painful foot conditions from wearing high heels, you should consult with your podiatrist right away.
Athlete’s Foot Relief and Prevention Tips
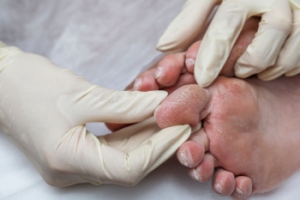
 Athlete's foot, or tinea pedis, is a common fungal infection affecting the skin of the feet, typically occurring between the toes. There are three main types of athlete’s foot, which are interdigital, moccasin, and vesicular. Interdigital athlete's foot typically occurs between the toes and is characterized by itching, scaling, and sometimes maceration of the skin. Moccasin athlete's foot affects the soles and sides of the feet, presenting as dry, thickened, and scaly skin that can sometimes crack. Vesicular athlete's foot features fluid-filled blisters, often appearing on the instep, and can cause intense itching and discomfort. The infection is caused by dermatophytes, which are fungi that thrive in warm, moist environments like locker rooms, public showers, and swimming pools. Risk factors include wearing tight, non-breathable footwear, sweating heavily, and walking barefoot in damp communal areas. Symptoms include itching, burning, peeling, and cracked skin, often accompanied by redness and blisters. Athlete's foot is extremely contagious and can spread through direct contact with infected skin or contaminated surfaces. Treatment involves antifungal medications, available as creams, sprays, or oral prescriptions, depending on the severity. If you have athlete’s foot, it is strongly suggested that you visit a podiatrist who can effectively treat the infection, which often includes prescribed medication.
Athlete's foot, or tinea pedis, is a common fungal infection affecting the skin of the feet, typically occurring between the toes. There are three main types of athlete’s foot, which are interdigital, moccasin, and vesicular. Interdigital athlete's foot typically occurs between the toes and is characterized by itching, scaling, and sometimes maceration of the skin. Moccasin athlete's foot affects the soles and sides of the feet, presenting as dry, thickened, and scaly skin that can sometimes crack. Vesicular athlete's foot features fluid-filled blisters, often appearing on the instep, and can cause intense itching and discomfort. The infection is caused by dermatophytes, which are fungi that thrive in warm, moist environments like locker rooms, public showers, and swimming pools. Risk factors include wearing tight, non-breathable footwear, sweating heavily, and walking barefoot in damp communal areas. Symptoms include itching, burning, peeling, and cracked skin, often accompanied by redness and blisters. Athlete's foot is extremely contagious and can spread through direct contact with infected skin or contaminated surfaces. Treatment involves antifungal medications, available as creams, sprays, or oral prescriptions, depending on the severity. If you have athlete’s foot, it is strongly suggested that you visit a podiatrist who can effectively treat the infection, which often includes prescribed medication.
Athlete’s foot is an inconvenient condition that can be easily reduced with the proper treatment. If you have any concerns about your feet and ankles, contact one of our podiatrists from Lexington Foot and Ankle Center, PSC. Our doctors will treat your foot and ankle needs.
Athlete’s Foot: The Sole Story
Athlete's foot, also known as tinea pedis, can be an extremely contagious foot infection. It is commonly contracted in public changing areas and bathrooms, dormitory style living quarters, around locker rooms and public swimming pools, or anywhere your feet often come into contact with other people.
Solutions to Combat Athlete’s Foot
- Hydrate your feet by using lotion
- Exfoliate
- Buff off nails
- Use of anti-fungal products
- Examine your feet and visit your doctor if any suspicious blisters or cuts develop
Athlete’s foot can cause many irritating symptoms such as dry and flaking skin, itching, and redness. Some more severe symptoms can include bleeding and cracked skin, intense itching and burning, and even pain when walking. In the worst cases, Athlete’s foot can cause blistering as well. Speak to your podiatrist for a better understanding of the different causes of Athlete’s foot, as well as help in determining which treatment options are best for you.
If you have any questions please feel free to contact our offices located in Harrodsburg, Frankfort, Georgetown, and Lexington, KY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Athlete's Foot
Athlete’s foot is an extremely contagious infection caused by a fungus that results in itching, burning, dry, and flaking feet. The fungus that causes athlete’s foot is known as tinea pedis and thrives in moist, dark areas such as shower floors, gyms, socks and shoes, commons areas, public changing areas, bathrooms, dormitory style houses, locker rooms, and public swimming pools. Athlete’s foot is difficult to treat as well because of the highly contagious and recurrent nature of the fungus.
Tinea is the same fungus that causes ringworm, and is spread by direct contact with an infected body part, contaminated clothing, or by touching other objects and body parts that have been exposed to the fungus. Because the feet are an ideal place for tinea to grow and spread, this is the most commonly affected area. It is, however, known to grow in other places. The term athlete’s foot describes tinea that grows strictly on the feet.
The most commonly infected body parts are the hands, groin, and scalp, as well as the feet. Around 70% of the population suffer from tinea infections at some point in their lives, however not all of these cases are athlete’s foot. Just like any other ailment, some people are more likely to get it than others, such as people with a history of tinea infections or other skin infections, both recurring and non-recurring ones. The extent to which a person experiences regrowth and recurrent tinea infections varies from person to person.
Sometimes people will not even know that they are infected with tinea or that they have athlete’s foot because of a lack of symptoms. However, most experience mild to moderate flaking, itching, redness, and burning. However, some of the more severe symptoms include cracking and bleeding skin, intense itching and burning, pain while walking or standing, and even blistering.
Because of the recurring nature of the tinea fungus and the athlete’s foot it causes, the best way to treat this condition is with prevention. You can take some preventative measures such as wearing flip flops or sandals in locker rooms and public showers to reduce contact with the floor. It also helps to keep clean, dry feet while allowing them to breathe. Using powders to keep your feet dry is a good idea, as well as keeping your feet exposed to light and cool air, to prevent the growth of tinea. If you do happen to get athlete’s foot, opt for using topical medicated creams, ointments or sprays. These treatments help eliminate and prevent it from coming back.
Choosing the Right Running Shoes for Your Needs

When it comes to running, selecting the appropriate footwear is essential for comfort, performance, and injury prevention. For long-distance running, cushioned shoes with ample support are ideal to absorb shock and reduce fatigue, enhancing endurance. Trail running demands shoes with rugged outsoles and superior traction to navigate uneven terrain and provide stability on rocky paths. If you are into sprinting or track running, lightweight shoes with minimal cushioning and a snug fit promote agility and speed. Cross-training shoes offer versatility for various activities, blending features suitable for running, jumping, and lateral movements. For those with overpronation or flat feet, motion-control shoes with reinforced arch support help correct gait imbalances and prevent injuries. Conversely, neutral shoes suit runners with normal pronation, offering balanced cushioning and support. If you have developed pain from wearing the wrong type of running shoes, it is suggested that you visit a podiatrist who can treat any foot ailment, and educate you about what type of shoes to purchase for your running style.
If you are a runner, wearing the right running shoe is essential. For more information, contact one of our podiatrists from Lexington Foot and Ankle Center, PSC. Our doctors can provide the care you need to keep you pain-free and on your feet.
Choosing the Right Running Shoe for Your Foot Type
To increase performance and avoid the risk of injury, it is important to choose the right running shoe based on your foot type. The general design of running shoes revolves around pronation, which is how the ankle rolls from outside to inside when the foot strikes the ground.
- Neutral runners are able to choose from a wide variety of shoes, including minimalist shoes or even going barefoot.
- Runners who overpronate, or experience an over-abundance of ankle rolling, should choose shoes that provide extra motion control and stability.
- Runners who underpronate, or supinate, have feet that have high arches and lack flexibility, preventing shock absorption. They require shoes with more flexibility and cushion.
If you have any questions please feel free to contact our offices located in Harrodsburg, Frankfort, Georgetown, and Lexington, KY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Choosing the Right Running Shoe for Your Foot Type
Running may seem like a simple to do. However, running is actually a complex movement that puts stress on the ligaments, bones, and joints of the body. Selecting the correct running shoe is important for increasing performance and avoiding risk of injury. Running shoes should be selected based on your foot type. Considerations such as trail versus road shoes are important. Your foot type dictates the degree of cushioning, stability and motion control you require. The most accurate way to learn your foot type is to visit a local shop that specializes in running shoes. Professionals can measure your arch type, stride and gait and help you with your shoe needs.
The design of running shoes is created around the idea of pronation. Pronation is the natural rolling movement of your ankle from the outside to inside when your foot strikes the ground. If you run properly you strike the ground on the outside of your heel and roll in the direction of your big toe before pushing off once more. Pronation is beneficial because it assists the lower half of your body in absorbing shock and storing energy. Those considered neutral runners pronate correctly and do not need running shoes that help correct their form. Neutral runners can choose from a wide variety of shoes, including barefoot or minimal types. However, those who have arch problems or who adopt an incorrect form while running may experience too much or too little pronation. They may require running shoes that offer additional support.
Those who overpronate experience an over-abundance of ankle rolling. Even while standing, those who severely overpronate display ankles that are angled inward. It is not uncommon for them to have flat feet or curved legs. The tendency to overpronate may cause many injuries. Areas that tend to become injured are the knees, ankles, and Achilles tendon. If you find that you have a tendency to overpronate, you should look at shoes that provide extra stability and motion-control. Motion-control shoes are straight and firm. Shoes of this type do not curve at the tip. The restricted flexibility along the middle of the shoe prohibits the foot from rolling too far inward as your foot strikes the ground.
A less common problem is underpronation. Underpronation, also called supination, is when the feet are unable to roll inward during landing. Those who underpronate have feet that lack flexibility and high arches. This prevents any kind of shock absorption, even though it does place less rotational stress on ankles and knees. This added force can cause fractures, ligament tears, and muscle strains because the legs are trying to compensate for the impact. Those who underpronate need shoes with more cushioning and flexibility. If you have a tendency to underpronate, selecting stability or motion-control shoes may cause you more problems by continuing to prevent pronation.